Childbirth is a miracle of nature. However, many times the miracle gets obscured by tragedy of fate, causing the childbirth to become a misfortune for the new-born baby and the expecting mother. This can occur due to many reasons – a birth defect in the baby being an important cause, which can suddenly change a happy occasion to a gloomy situation. Fortunately, another miracle – the marvel of modern science, has restored hope in many, otherwise sad cases. The procedure in this context is, Fetal Surgery – Surgery to correct the medical anomalies of a baby, while he/she is still in mother’s uterus, before being born.
The traditional approach that most of the health professionals follow for congenital defects of babies, is planned delivery at term, followed by repair/treatment of the problem of the new born, in a centre with facilities, to handle such kind of problems. But the downside of this approach is that, the baby may not survive that long, to benefit from this kind of procedure. Congenital birth defects are a major cause of morbidity & mortality in infants. The compelling reason for undertaking this kind of surgical intervention is the belief, that the disease affecting the foetus will not allow it, to survive till delivery or the baby would succumb soon after birth. Foetal Surgery gives hopes to these babies, who otherwise would never survive long enough to see the world.

Fetal Surgery is rather a new development, in the field of medicine & is also known as – prenatal surgery/antenatal surgery or Fetal reconstructive surgery. All these are basically the same thing and helps by surgical remedy of birth defects of foetuses in pregnant uterus. This modern form of treatment is unknown to a vast majority of people and facilities for this kind of care is also available in few select centres only. The reason for this would become clear, by the following discussion.
The Hindu Epic – Mahabharata, written thousands of years ago, has an interesting anecdote, that resembles modern day Foetal Surgery. It is said that in the great war of Mahabharata, between the good guys (Pandavas) and the bad guys (Kauravas), all the Kauravas and their descendants had died by the end of war, and the same happened with the Pandavas, with only the main Pandava princes and a single pregnant daughter in law surviving. In this critical juncture, Ashwatthama – last surviving ally of the Kauravas, tries almost successfully to kill the male child in womb of the daughter in law. However, due to timely actions of Lord Krishna (who is human manifestation of a divine god), the baby in uterus is brought back to life and later is born as a healthy baby – prince Parikshit, the only surviving descendant of the Pandava clan.

The beginning of Foetal surgery is linked to finding a cure for foetus, whose life was endangered due to Rh incompatibility. Here it would be helpful to mention that Rh incompatibility is a serious condition that can arise, when a woman with Rh negative blood group, carries a baby with Rh positive blood group (usually a second or later pregnancy of the woman). The baby in uterus may face haemolytic anaemia in this case (where its red blood cells are destroyed), if the Rh antibodies from mother, reaches the baby through the placenta. For treatment of this condition, foetal blood transfusion done through mother’s abdomen & uterus into the foetus’s abdomen (a procedure known as intraperitoneal transfusion), was first done by Sir William Liley in 1963, establishing him as the father of foetal surgery.
However, the modern version of Foetal Surgery started sometime later in 1981 in University of California, San Francisco, when the first successful open foetal surgery was done for Congenital Hydronephrosis. In this condition the blockage of Urinary tract, causes the kidney to dilate and enlarge in size. Since that time many more diseases and many other techniques, have been included in the spectrum of foetal surgery.
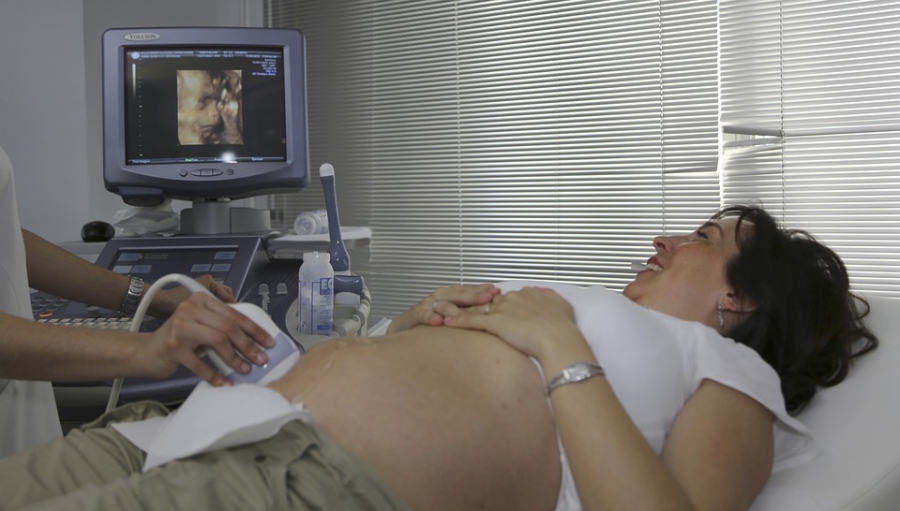
An integral part of this procedure, is the diagnosis of the health problem, in the developing baby in mother’s womb. In this context, the role of Ultrasound is very important. The widespread availability at a low cost, which enables the radiologist to diagnose many anomalies in the developing baby in the womb, has made many to consider it as a first diagnostic modality in these situations.
The further innovation and developmental modifications, in form of transvaginal ultrasound, 3D and 4D technology has made the scope of this diagnostic modality, applicable to much broader spectrum of medicinal problems. The main among these are – craniofacial, skeletal and neural tube anomalies. Measurement of Lung volume, for judging lung developmental abnormalities & evaluation of congenital heart defects are some other applications. Ultrasound has also helped during the actual surgical procedure, where it has helped in identifying foetal anatomical landmarks and evaluating overall foetal condition.
However, in certain situations, Ultrasound may be not be able to show the greater picture. In this situation – Ultrafast MRI technology can be a diagnostic procedure, that gives a better evaluation. This is due to a better field of view, a more precise volumetric measurement and a better soft tissue contrast. It is especially beneficial in diagnosing abnormalities of lung development and other thoracic growths.
Before undertaking foetal surgery, it is important that certain criteria’s, as decided by International Foetal Medicine and Surgery Society, should be fulfilled. It should be done only in a centre, where highly trained doctors of different branches of medicine, like; radiologists -well versed with ultrasound studies, anaesthesiologist’s - expert in handing complicated delivery cases, paediatric surgeons and neonatologists are easily available. The hospital should have an ethics committee, to supervise and help the patient’s relatives in taking an informed and balanced decision, in choosing the surgical intervention.

Before undertaking the surgery, the diagnosis should be established beyond doubt, including ruling out other conditions, that may make the surgery a dangerous proposition. The disease which necessitates surgery should be well understood by all the health professionals involved. The risk of undertaking surgery should be well justified, and the absence of better & easier satisfactory treatment of the child after birth, has to excluded first. The procedure should carry minimum risk to the mother & historical precedent of improvement of baby’s condition by surgery should be present.
Grossly speaking there are two different methods available.
Open Foetal Surgery is somewhat similar to Caesarean section, in the sense that a surgical incision is placed on lower abdomen of the mother, followed by another incision on the uterus (a procedure, which is surgically known as hysterotomy) and approach to foetus enabled. The difference with Caesarean procedure, however lies in the fact that, during the procedure, continuation between foetus and placenta is maintained & foetus is returned back to Uterus after completion of the foetal surgery procedure.
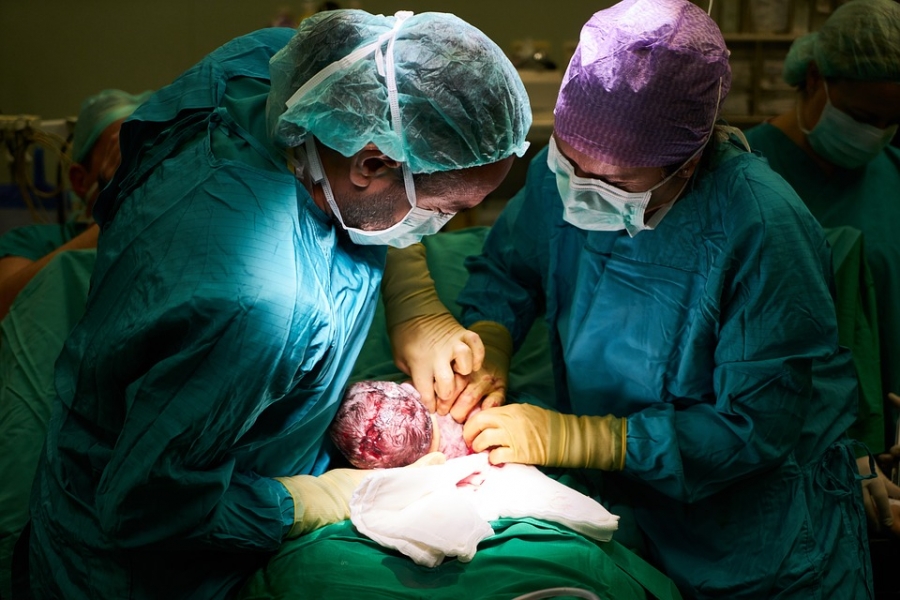
During the procedure warm Ringer Lactate solution is used to continually infuse the Uterus. In the end, surgical incisions on the uterus & abdominal wall of the mother are closed, after replacing lost amniotic fluid by warm Ringer Lactate solution. Medicines known as Tocolytics, are also administered to the mother to prevent premature delivery. Following surgery, the mother is kept in the hospital for another 3 to 7 days for recovery, before being discharged for going home.
Endoscopic method for foetal surgery was developed in the 1990s. The procedure is usually done on the 2nd or 3rd trimester of pregnancy. This enabled the approach to foetus by very small incision and instruments, directly from the mother’s abdomen (and uterus) & through the amniotic cavity. An important advantage is that, the whole surgical procedure is visible in a television monitor. Sometimes, sonographic visualisation on separate screen by concomitant ultrasound gives much better visualization and understanding of the foetal situation.
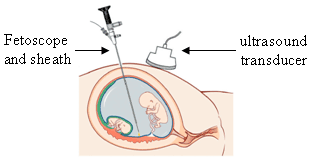
As this procedure is less invasive than Open Foetal Surgery, so the mother’s recovery is much faster and chances of later preterm onset of labour is decreased (however preterm labour may still occur, necessitating careful monitoring). On the downside, the surgical expertise needed for this kind of surgery is much more complicated, than the open method discussed earlier.
This denotes some well-defined systematic procedures, that is followed at the time of final delivery of the baby, who is believed to be suffering from life threatening airway obstruction. This is done in cases, where the breathing abilities of the new-born babies are insufficient on their own, due to faulty airway or some obstruction & additional external support is anticipated. This kind of delivery can only be done in a hospital having properly trained & experienced – Gynaecologist, Anaesthetist, Paediatric surgeon and neonatologist. The delivery is done like Caesarean section, with administration of general anaesthesia, to ensure full relaxation of the Uterus.
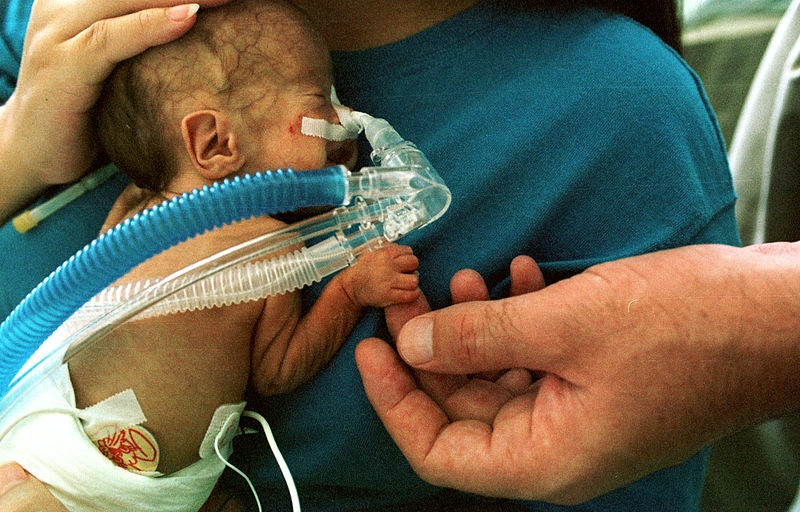
At the time of delivery and before the new born is separated from the placenta, bronchoscopy of the baby is done, to evaluate the respiratory tract. If possible an endotracheal tube, is passed to the baby’s trachea through the mouth & breathing given to the baby. If breathing is established with this measure, then only then the umbilical cord is cut & the infant is delivered. If it is not possible to pass endotracheal tube, through the mouth due to some obstruction, then a tracheostomy is done by cutting open the trachea in the neck, below the obstruction, and a tracheostomy tube inserted. Only when the airway is restored and breathing is satisfactory, the new born is separated from umbilical cord, delivered and shifted to paediatric intensive care unit for further evaluation and management.
Rapidly advancing medical knowledge and facilities have created unbelievable miracles in modern medicine, with many diseases which were without much treatment previously, now amenable to satisfactory treatment giving productive life to the individual.
Some of the health conditions which can be satisfactorily treated by Open Foetal Surgery are –
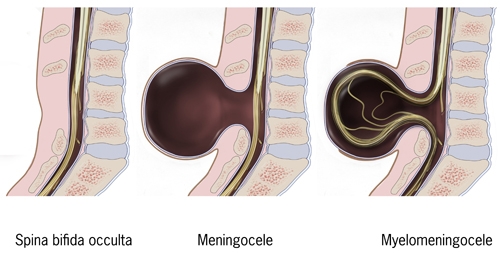
The embryonic neural tube does not close properly, giving rise to abnormalities in the nervous system, as the developing spinal cord and brain is directly exposed to the amniotic fluid. Although the basic pathology (problem) may be the same, but different manifestation causes a spectrum of disorder. One of the treatable forms of this disorder is – myelomeningocele, the correction of which by open foetal surgery, gives much better results, than opting for the surgery after birth.
This involves a defective heart structure, which manifests itself from the time of birth. Some specific varieties of Congenital heart defects, respond to open foetal surgery.
This is a congenital defect that presents in children, and is associated with abnormality in Lung development.
This is a tumour that develops in the base of tailbone, seen in young children. Though the vast majority are benign and harmless, but rarely harmful cancerous growth can occur.
The disease conditions which can be treated with Endoscopic Foetal Surgery are –
This birth anomaly is characterised by defects in the spinal cord and in the bones of the spine. This again can be of different types - depending on size, location, type of defect and complications. Here minimally invasive foetal surgery is undertaken for the closure of malformation, producing the defect. This benefits the baby a lot, while causing minimal harm to the mother.
Also known as feto – fetal transfusion syndrome, the blood supply of twin foetuses (monochorionic twins) can become connected in this condition, due to sharing of single placenta. This allows the blood to pass from one twin to other, which can lead to serious complications on both foetuses. Laser ablation of vessels, by minimally invasive foetal surgery is a good treatment option.
This is a tumour of Placenta, which if, is large in size or are multiple in number, can lead to several complications. However, laser occlusion of blood vessels by Fetoscopy is an effective solution.
This is a spectrum of disorder characterised by birth defect of the diaphragm and can lead to life threatening complications. Endoscopic foetal surgery has been found to be helpful in some cases.
As mentioned before, only a handful of people in society, have the knowledge about this subject. The required diagnostic modalities are not available in all places, for the preliminary diagnosis of the medical anomalies. Only a few select centres have the technological expertise and multidisciplinary teams available for successful surgery of the foetuses. Ensuring maternal safety, during and after surgery in the foetus are of paramount importance. However, surgical opening of the uterus, made at the time of foetal surgery, can sometimes cause problems in future pregnancy.
Many times, babies undergoing foetal surgery are born preterm, so this factor should be kept in mind at the time of delivery. Caesarean procedure is done for mothers who previously had open foetal surgery cases, but however may not be required in cases treated by endoscopic foetal surgery. This risk is increased many folds, if the mother is a smoker, or is very young or very old in age & evidence of multiple gestation is present. Open Foetal Surgery cases may sometimes cause complications like – amniotic fluid leaks, chorioamniotic separation and pulmonary oedema in mother. In spite of all sincere efforts, chances of perinatal mortality are always present, more so in the case of open surgical procedures. Even after birth, the baby may require addition reconstructive procedures, for a normal function and appearances.
Foetal Surgery is a modern surgical technique devised to correct the birth defects of a developing baby in mother’s uterus, before birth. However, majority of the people are still unaware of this medical miracle. The requirement of multiple super specialization branches of health professionals, along with complicated gadgets is the cause, that centres for this kind of surgery are very limited. However, as the information about the procedure increases with time, it is hoped that centres for such kind of surgery would also grow exponentially, as more and more diseases comes into the purview of foetal surgery. Foetal surgery becomes all the more important in the face of the fact that - nothing more is important or more fulfilling, than to save the life of a baby, who is yet to be born.
(Disclaimer – This short article is just to raise general public awareness about this novel modality of treatment and is certainly not a substitute for a direct individualised face to face consultation with a registered medical practitioner. The scope of Foetal Surgery goes much beyond the short description given here, so people contemplating about the procedure, should consult an expert first, before taking any final decision.)