Modern medicine has brought forward many modern-day miracles, which has given a new lease of life, to many people who had given up all hope. One of such issues concerned is becoming a mother, which is a very common innate desire of all women. However, not all women are lucky enough to have fulfilment of this primordial instinct and female infertility is a leading health problem nowadays.
The cause of female infertility is many, and the treatment is directed towards specific cause. A recent statistical survey showed that, 15 percent couples of reproductive age group suffer from the problem of infertility. Birth defects are responsible for causing absence of uterus in around, 1 in 500 women, in general population. Many women also have their uterus removed due to some health problem. As must be obvious, without a healthy uterus, a woman cannot have a successful pregnancy, and becomes infertile.
Previously only option available for the women, lacking uterus but desirous of having a child, was adoption from orphanages or having a child through a surrogate mother. However, Uterus transplant has changed radically the entire scenario, in recent years. This treatment has helped many women to again have hopes of a successful pregnancy.
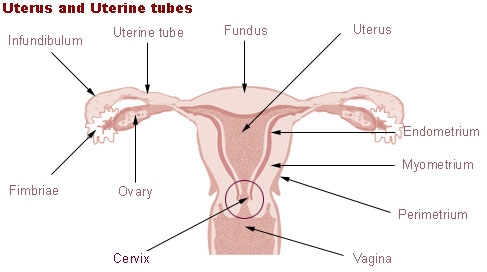
In Uterus Transplant, a surgical procedure is undertaken, where a healthy uterus is taken from another woman (who may be living or dead) and transplanted into a woman, whose uterus is either diseased or totally absent. The surgical procedure establishes connection of recipient’s veins & arteries, ligaments and vaginal canal to that of the donated uterus and its corresponding parts.
The attempt for a successful uterine transplant in humans, started many decades ago, in the 20th century. After initial attempts in animals, trials were done in humans, but these met with tragedies, as most early medical experimentations usually do. As alternate options for female infertility treatment, in form of In Vitro Fertilisation (IVF) and surrogacy developed, the preference tilted towards the mentioned procedures.
In recent times, interest on this surgical procedure was rekindled, at the turn of 21st century; when a 26-year-old woman received a uterus removed from another 46-year-old woman, in the year 2002 in the Kingdom of Saudi Arabia. The woman, who received the transplanted uterus, had initially 2 menstrual cycles afterwards; but 3 months later complications related to the procedure developed and ultimately, the transplanted uterus had to be removed.
Another turning point was the first uterus transplant from a dead woman into a living, which was done on 2011 in Turkey. The 21-year-old Turkish woman, recovered from the procedure and started having her periods. However, in the year 2013, after 8 weeks of pregnancy, the patient had her pregnancy terminated, when examinations showed that the baby in her womb had died.

Afterwards, uterus transplant was attempted in different parts of the world, with various degrees of success. It was during these years that, mother to daughter uterus transplant was undertaken in many countries, situated far and wide, and included the developed countries like – Sweden (first of the kind in 2012), to the developing countries like India (in the year 2017).
After years of hard work and multitude of attempts, successful result in Uterus transplant with a successful childbirth was finally obtained. The case was reported by the British medical journal – Lancet, which described the birth of a healthy baby boy, in September 2014 to a 36-year-old Swedish woman, who had received a uterus transplant, from a 61-year-old woman, a year before.
The woman was born with a rare birth defect, in which although the ovary was present, but the uterus was absent. As she was desirous of having a baby, her egg was fertilised with her husband’s sperm, as a part of in vitro fertilization (IVF). The resulting embryo was implanted into the transplanted uterus, in the woman’s body. Immunosuppressive drugs were used to prevent rejection of this foreign organ. In spite of this, mild rejection episodes occurred, which by god’s grace could be controlled by medication.
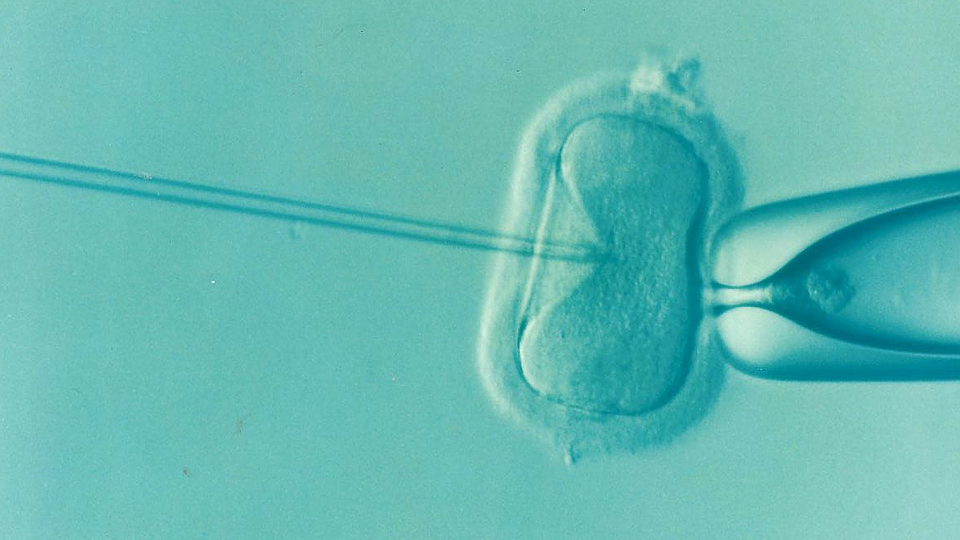
Although the delivery was done by a caesarean section, at 32 weeks of pregnancy (the mother had developed high blood pressure during pregnancy), the baby weighing 1.8kg was otherwise normal, and correspondingly similar to that of other babies delivered at that gestation period.
An event from December 2017, created quite a ripple in the medical fraternity. The news declared the first successful pregnancy, in a case of uterine transplant, where the organ was taken from a deceased donor. The pregnancy involved a team of doctors from Sao Paulo – Brazil, where a 32-year-old woman, who lacked a uterus due to a birth defect, had received uterus transplant on 20 September 2016; where the organ was harvested from a 45-year-old woman, who had expired due to cerebral haemorrhage. She had been a mother of 3 children (all normal vaginal birth) and her blood group of O+ve, was the same as the woman receiving the uterus.
Months before the transplant procedure, the woman’s egg and her husband sperm were fertilized artificially, via in vitro fertilization (IVF) procedure, and 7 months after the transplant (when the woman was found to have menstruated and was in stable condition), the embryo (which was cryopreserved) was implanted into the uterus. The pregnancy was uneventful and a baby girl, weighing 6 pounds, was delivered by Caesarean section on Dec 15, 2017 after 35 weeks of pregnancy. The transplanted uterus was also removed during the caesarean section, so the mother could be taken off immunosuppressants.

One of the facts which made the first successful childbirth, in a case of Uterus Transplant where the organ was taken from a deceased woman, was the fact that the donor uterus had survived for 8 hours, without oxygen (and absent blood flow), but still gave the desired result perfectly.
Before the trend of harvesting uterus from dead women started, organ was harvested from living women, usually friend or family members of the woman desiring to have a baby. But the donor had to undergo a major surgical procedure, known as – Radical Hysterectomy, which can take anywhere between 3 to 4 hours to perform and has its own set of complications. These can be totally avoided by harvesting uterus from a dead woman.
People are far more likely to be willing to donate their organs, after death than at a time when they are still alive. This would make available a much greater amount of donor population, making the uterus transplant procedure, available for many more women, desirous of the procedure.
It has to be mentioned that Uterus transplant can only be done, if certain preconditions are met. The donor female should be of reproductive age, must have completed her family, should be of sound mind and donating her uterus on her own free will. She should not have any medical or surgical contraindication for the mentioned procedure.
The recipient woman should not have any other health problem, that is a contraindication for the procedure; she should be having the procedure on her own free will and only after failure or unavailability of simpler options. She also should be physically strong and mentally mature, to comply with medical instructions and understands the risk of the procedure along with responsibility of motherhood.

The medical team is also subjected to certain criterion of standard maintenance, including skill and technical expertise and infrastructure backup. Strong moral, legal and ethical practices, including the professional obligations of maintenance of privacy of the patients and no conflict of interest are mandatory.
The procedure is not just costly (and not covered by insurance), but the surgical expertise and technical skills and infrastructure needed for the supervision of the organ donor, recipient (& the expectant mother) and the baby developing in the womb; makes only a few select centres suitable for these kinds of major interventions.
The surgical interventions needed for the procedure, is not just one or two; but a total of 3 procedures. These include – Harvesting Uterus from an organ donor & transplanting it into a recipient lacking normal uterus, Caesarean section for delivery of the baby and finally the 3rd surgery for removing the transplanted uterus, after 1 or 2 successful pregnancies (which is usually done during the Caesarean section). This is done, so that the woman who received the transplanted uterus (the organ recipient), could stop taking immunosuppressive drugs (which have to be continuously taken, to prevent organ rejection and these certainly have serious side effects) after completing her family.
The immunosuppressant drugs that a woman has to take, to prevent rejection of the transplanted uterus, can cause serious adverse effect, and the patient has to stay in constant medical supervision, along with repeated investigations undertaken in a regular basis in a periodic interval.

The problems of harvesting organ for uterus transplant from living donors has already been mentioned previously, but taking the organ from a deceased woman, has also its share of problems. The surgeons are hard pressed for time, during this procedure. Besides the practical difficulty in obtaining an organ and accompanying technical challenge of the harvest, matching of the blood group, completion of the procedure before the lack of blood supply cause deleterious effect on the donor uterus; are some of the challenges, which have to be taken care of.
21st century has heralded a new era in not just modern medicinal marvels, but also a new perspective at looking at social justice and human equality. In this context, betterment of life for people with physical abnormalities have emerged as a prominent factor, towards which fruits of medical advance have been directed. The ability to live a life of dignity and avail the simple pleasures and benefits, that all humans deserve, has shifted the focus on Uterus transplant and pregnancy in Transgender women desirous of having children.
In spite of all the good intentions, the actual decision to undertake such a surgical manoeuvre, would encounter multiple problems, specially because of the anatomical and physiological abnormalities in the person concerned. The correction of all these abnormalities are surely not an easy or a single step procedure. Before undertaking Uterus Transplant in these patients, other preliminary procedures would be needed. These would include – hormone replacement therapy and gender (sex) reassignment surgery.

The Uterus Transplant procedure would also be needed to be modified to, Utero- Vaginal Transplant, where more than normal (as much as possible) donor vagina have to be taken. The donors in this case would be only the dead (deceased) women and certainly not living women, for obvious reasons. After stabilisation of the surgical results and only after ruling out serious side effects of immunosuppressant drugs, can pregnancy be attempted. At the time of birth of child, Caesarean section would also be needed for safe delivery, followed by removal of the uterus, like other cases.
The increase in surgical procedures, translates into an increased probability of manifestation of possible complications of these surgical manoeuvres. The legal protocols for undertaking these kinds of procedures are not favourable in most countries of the world. All these factors would have to be overcome, before a transwoman gives birth to a healthy baby.
As of December 2018, 56 transplant procedures of the kind mentioned above have been done (with almost half the number, in countries of Europe) and 13 successful childbirths have taken place. Although this number would surely increase in coming years, but as of now, Uterus Transplant is still a new procedure in majority of the countries worldwide. Clearly more study and experience are needed before it can be routinely used across the globe.
(Disclaimer – This article is just for raising awareness in the public about Uterus Transplant procedure, and is certainly not a substitute for a face to face consultation with an experience registered Gynaecologist in your area. Uterus Transplant is an evolving procedure and it is quite possible, that we would see many changes in the coming years. Legal formalities are different across the world, when it comes to practical implementation of recently invented medical procedures. Readers discretion is advised.)